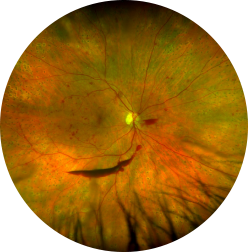
What is Diabetic Retinopathy?
Patients with Diabetes Mellitus (DM)can have abnormal blood sugar levels and this can affect the retina in many ways. In Diabetic Retinopathy (DR), the retinal blood vessels are damaged. Diabetic retinopathy can affect Type I or Type II diabetics.
There are three main ways that diabetic retinopathy causes vision loss: diabetic macular edema, proliferative diabetic retinopathy and poor perfusion of the retina due to lack of normal blood flow (Ischemia).
Diabetic Macula Edema (DME):
Non-Proliferative Diabetic Retinopathy (NPDR)or Background Diabetic Retinopathy (BDR)describe initial stages of diabetic retinopathy. Blood vessel damage in diabetic retinopathy can lead to abnormal leakage of fluid and blood into the retina; this leakage can cause the retina to swell. If this leakage occurs in the macula, it is called Diabetic Macular Edema (DME). This is the most common cause of visual loss in patients with diabetes and ranges from mild to severe.
Proliferative Diabetic Retinopathy (PDR):
Proliferative Diabetic Retinopathy (PDR)occurs when abnormal blood vessels grow from and on top of the retina. These abnormal blood vessels are fragile and can bleed into the eye causing a Vitreous Hemorrhage. This can cause dark floaters and may cause immediate loss of vision. Pulling and contraction of these abnormal vessels and their associated scar tissue can lead to a Tractional Retinal Detachment, where the retina is pulled away from the back of the eye leading to loss of vision.
What is the treatment for Diabetic Retinopathy?
Medical treatment may involve the use of injections of medicine into the eye (Intravitreal Injections) to treat diabetic macular edema. Recent science has shown that DME and PDR are controlled by a signal sent from the damaged retina called Vascular Endothelial Growth Factor (VEGF). Several VEGF blocking drugs (including Avastin, Lucentis, and Eylea) and other medications (steroids and steroid implants) when injected into the eye can cause DME and PDR to regress. Most of these agents provide only temporary relief and need to be given repeatedly over a prolonged period of time.
Laser Treatment may be recommended for people with DME, PDR, or severe NPDR. The main goal of treatment is to prevent further loss of vision. The laser is applied to the damaged retina to shrink the abnormal blood vessels and prevent them from growing. Multiple laser treatments may be necessary. This is not a curative procedure and does not always prevent further loss of vision.
Surgical treatment, Vitrectomy,may be recommended if bleeding from diabetic retinopathy causes a vitreous hemorrhage and associated vision loss. Additionally, surgery may be needed to treat tractional retinal detachment in the setting of extensive blood vessel and scar tissue growth.
Although we can’t prevent the occurrence of diabetic retinopathy, good medical control and early diagnosis and treatment can significantly reduce the progression to severe visual loss. This requires close cooperation between the primary physician, ophthalmologist and patient. Optimal blood sugar, blood pressure, cholesterol and weight control can reduce the long-term risk of vision loss from diabetic retinopathy. The primary physician not only plays a key role in medical management, but assumes responsibility for patient education and coordination of care. Early detection of diabetic retinopathy allows the best chance for maintaining good vision.